Pregnancy advice in 2026 can feel nonstop. One week you are hearing about prenatal vitamins. The next week it is blood pressure, vaccines, or sleep. Then someone on social media starts talking about wearable health tech and asks a question that sounds very reasonable: if a continuous glucose monitor can track glucose all day, why do I still need the glucose drink test during pregnancy?
That question is getting more attention for a reason. Many moms already use wearables before pregnancy. Some track sleep, heart rate, workouts, and stress. Others are now hearing about continuous glucose monitors, often called CGMs, from friends, online communities, or providers. It makes sense to wonder whether a CGM could do the same job as the standard gestational diabetes screening test.
In most pregnancies, the answer is still no. A CGM can be useful in some situations, but it does not automatically replace the glucose drink test that many providers still use between 24 and 28 weeks. That does not make CGM useless. It just means the two tools do different jobs. If you understand that difference, the whole topic becomes much less confusing.
If this conversation feels familiar, it may help to start with our post on gestational diabetes in 2026 and why the 24-to-28 week test still matters. This article goes one step further by focusing on the tool many moms are asking about now: CGM.
Why more moms ask about wearables instead of the glucose drink
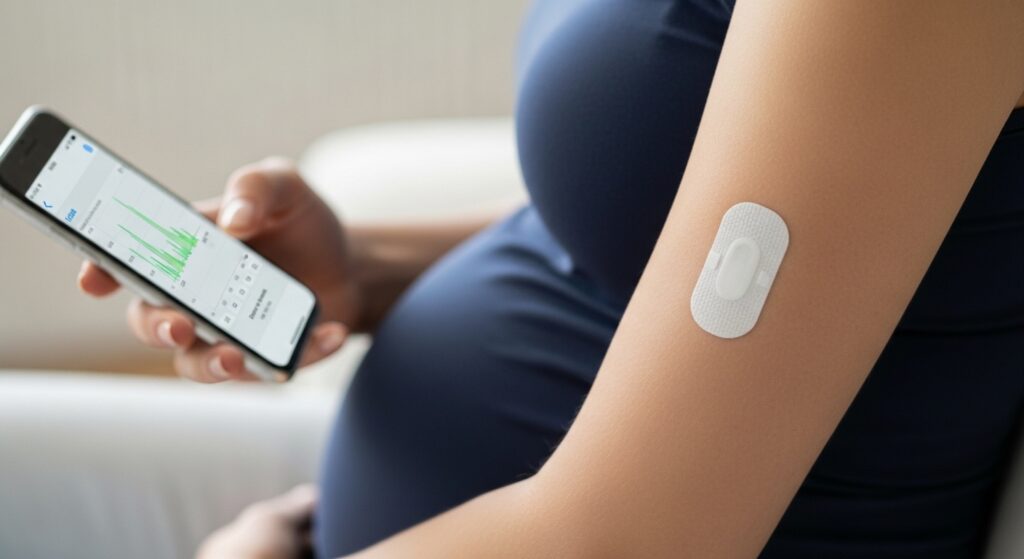
Part of the interest comes from convenience. The glucose drink test can feel annoying, stressful, and overly medical. A wearable sounds easier. You place a small sensor on the body, connect it to an app, and get numbers throughout the day. That feels more modern than drinking a sweet liquid in a clinic and waiting for blood draws.
Another reason is that pregnancy health has become more data-driven. Moms are already hearing about blood pressure tracking, symptom tracking, and wearables. If you read our article on smartwatches in pregnancy in 2026, you have already seen this shift. People want more real-time information. They want tools they can use at home. They also want fewer surprises at prenatal visits.
What a CGM can do day to day
A CGM tracks glucose trends over time. Instead of giving you one isolated number at one appointment, it shows patterns. You may see how your glucose changes after meals, overnight, or during a more stressful day. That can be very helpful for someone who already has diabetes, for someone whose provider wants closer glucose monitoring, or for someone trying to understand how food choices affect their body.
That pattern-based view is the biggest strength of CGM. It can show what happens in real life, not just what happens during one test. In pregnancies already complicated by diabetes, that kind of day-to-day information can help guide treatment and follow-up.
What the standard glucose drink test measures differently
The glucose drink test answers a more specific screening question. It is designed to show how your body handles a known glucose challenge under standardized conditions. That matters because a clinic-based screening test gives providers a defined way to compare results against established pregnancy thresholds.
In plain language, the glucose drink test is not trying to show your whole daily pattern. It is testing how your body responds to a set amount of glucose in a structured way. That is why the test still holds a central role in screening for gestational diabetes. It is standardized, familiar to providers, and tied to current diagnostic pathways.
What current guidance says in 2026
This is where the answer gets clear. Current diabetes guidance still does not treat CGM as a replacement for screening or diagnosis. The American Diabetes Association’s 2026 Standards of Care states that there is not enough evidence to support CGM for screening or diagnosis of diabetes. In other words, CGM may help with monitoring, but it is not the same as the test your provider may use to diagnose gestational diabetes.
That point matters because online advice often blurs the line between monitoring and diagnosis. They are not the same. A tool can be helpful without replacing the formal test. The World Health Organization also added more attention to diabetes during pregnancy by launching its first global guidelines on the topic in late 2025, which shows how important glucose management has become in maternity care.
So if you are hearing more about CGM in pregnancy 2026, that interest is real. The question is not whether CGM is interesting or promising. The question is whether it can fully replace the glucose drink test in a routine pregnancy right now. Based on current guidance, that answer is still generally no.
If you are early in pregnancy and this topic is already on your mind, you may also want to review our guide on when to schedule your first prenatal visit in 2026, because early visits are often where screening plans start to take shape.
How to decide what makes sense for your pregnancy
Questions to ask your prenatal provider
The best next step is not guessing. It is asking better questions. If you are curious about CGM, bring it up directly at your prenatal visit. Do not need a complicated speech. Can ask, “Would a CGM help in my pregnancy, and would I still need the standard gestational diabetes test?” That question gets to the point fast.
You can also ask whether you have any personal risk factors that make earlier testing or closer monitoring more likely. Some moms need a straightforward routine screen later in pregnancy. Others may need a more personalized plan based on medical history, prior gestational diabetes, or current symptoms. The right answer depends on your pregnancy, not on what worked for someone else online.
When CGM may still be useful during pregnancy

Even when it does not replace the screening test, CGM may still help in some cases. A provider may use it when someone already has diabetes, when glucose trends need closer follow-up, or when extra data could support a treatment plan. That is why this topic is not black and white. The issue is not whether CGM has value. It clearly can. The issue is whether it can stand in for the formal screening pathway by itself.
This is similar to other home tools in pregnancy. For example, home blood pressure tracking can be helpful, but it does not replace medical judgment. Our article on home blood pressure monitoring in pregnancy in 2026 makes that same point. Home data can support care. It does not automatically replace clinical screening or diagnosis.
What to expect if you still need the 24-to-28 week test
If your provider recommends the usual gestational diabetes screening window, that does not mean your questions were wrong. It just means they are following the current standard approach. The goal is to catch a condition that can show up even when you feel fine. That is one reason gestational diabetes can surprise people.
Try to approach the test as useful information, not as a judgment on your health habits. If the result is normal, great. If it is not, finding out early gives you and your care team more time to respond. In many cases, earlier clarity lowers stress because you stop guessing and start planning.
It may also help to keep your bigger pregnancy picture in mind. Sleep, food, symptoms, appointments, and screening can all pile up fast. If you feel overwhelmed by all the advice, our article on nutrition myths in pregnancy may help you sort solid information from noise.
The bottom line is simple. CGM in pregnancy 2026 is a timely topic because wearable health tech is getting more attention, and many moms want easier ways to understand glucose. But current guidance still separates CGM from formal screening and diagnosis. A CGM may help with monitoring in the right situation, yet it usually does not replace the glucose drink test on its own.
If you are wondering what applies to you, bring the question to your prenatal provider. Ask what they recommend, why they recommend it, and whether CGM has any role in your care. That conversation will be more useful than any one-size-fits-all answer online.
For evidence-based reading, you can review the ADA 2026 Standards on diagnosis and classification of diabetes, the WHO guidance launch on diabetes during pregnancy, and the CDC overview of gestational diabetes.
Medical disclaimer: This article is for educational purposes only and is not a substitute for personal medical advice. Always talk with your OB-GYN, midwife, or prenatal care provider about what is right for your pregnancy.



